Medical equipment financing allows doctors to acquire expensive clinical tools without draining working capital. Because high-quality diagnostic, surgical, and imaging equipment can cost anywhere from $20,000 to several million dollars, most physicians use structured financing rather than paying cash.
The smartest medical equipment financing strategies:
- Match equipment cost to projected patient revenue
- Choose between loans and leases based on technology life cycle
- Protect cash flow, especially during insurance reimbursement delays
- Use tax strategy (Section 179, depreciation) to reduce effective cost
When done correctly, medical equipment financing is not debt—it’s a growth lever. When done poorly, it becomes a long-term burden that restricts your practice’s flexibility.
Why Doctors Finance Medical Equipment
Modern medicine runs on technology. Whether you’re in primary care, cardiology, dentistry, dermatology, orthopedics, or surgery, your ability to diagnose and treat patients depends on equipment that is increasingly advanced—and expensive.
A single imaging machine can cost more than a home. Even smaller tools like exam tables, autoclaves, and monitoring systems add up quickly when opening or expanding a practice.
For example:
- An ultrasound system can range from $25,000 to $100,000+
- A digital X-ray unit may cost $60,000 to $250,000
- An MRI system can exceed $1 million
- Dental chairs and imaging systems often total $100,000+ per operatory
Because of these costs, medical equipment financing is standard practice across the healthcare industry. Hospitals, private practices, ambulatory surgery centers, and specialty clinics all rely on structured financing to acquire equipment while maintaining operational stability.
Financing allows doctors to:
- Preserve cash reserves
- Smooth out payments over time
- Align equipment cost with revenue generation
- Upgrade technology without massive upfront capital
This is particularly important in systems where reimbursement cycles are delayed—like Medicare and private insurance in the United States.
Organizations such as U.S. Small Business Administration support physician-owned practices through loan programs, and many banks specialize in healthcare lending.
The key is understanding what equipment doctors typically finance—and how to do it intelligently.
Medical Equipment Doctors Commonly Finance Diagnostic & Imaging Equipment
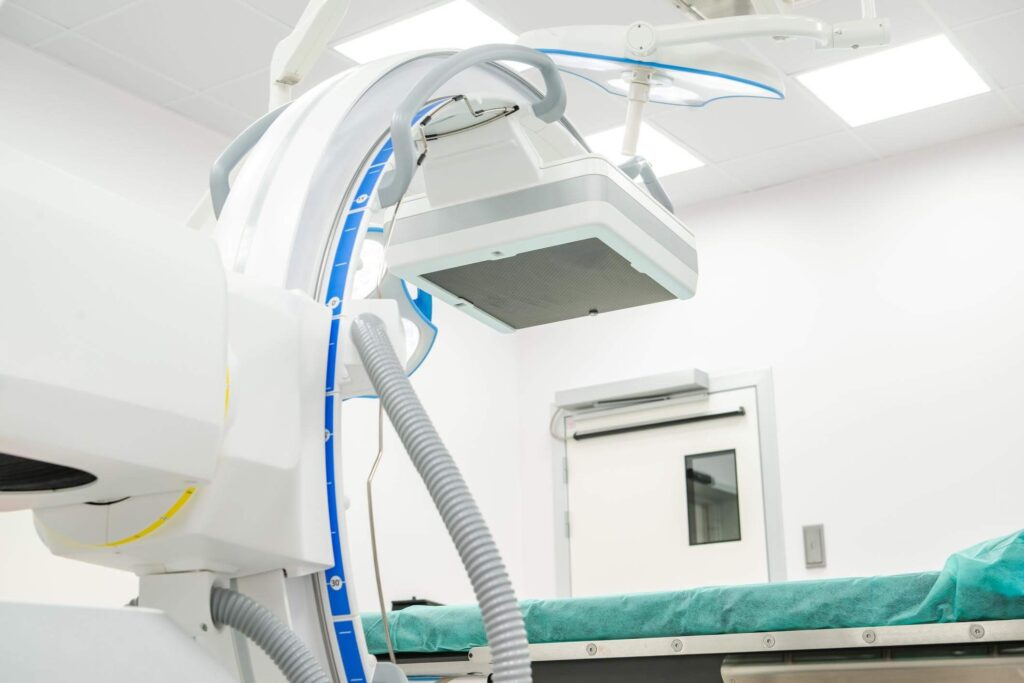
Diagnostic equipment is one of the most commonly financed categories in healthcare.
Examples include:
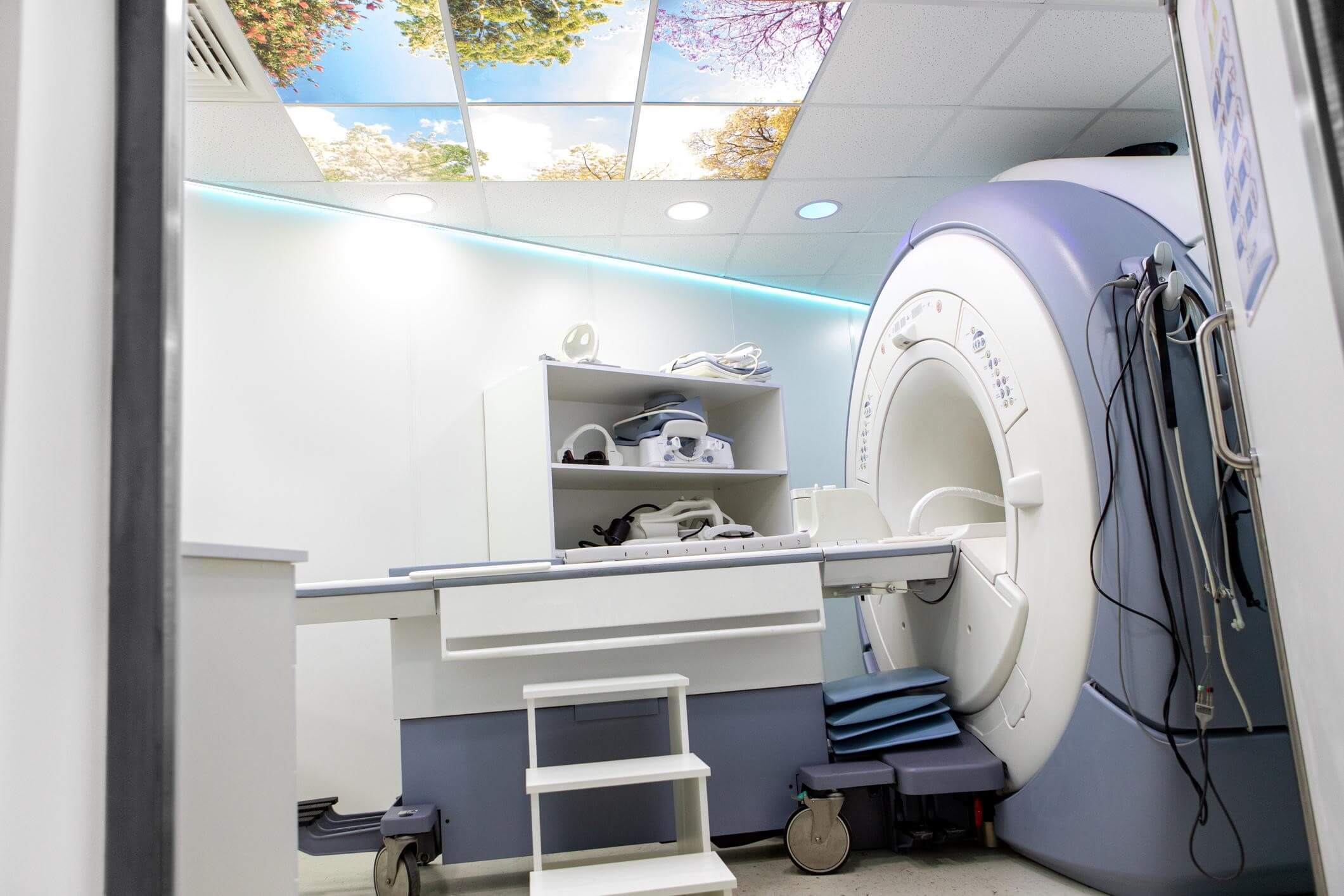
- MRI systems
- CT scanners
- Ultrasound machines
- Digital X-ray units
- Mammography systems
Why finance instead of buy?
- High upfront cost
- Revenue generation potential
- Rapid technological upgrades
Imaging equipment financing is often structured over 5–7 years because the equipment generates billable procedures that offset monthly payments.
For large purchases, physicians may use healthcare-specific lenders or banks with medical divisions. Some imaging manufacturers even offer in-house financing programs.
Medical equipment financing for imaging is often the single biggest debt obligation in private practice outside of real estate.
Surgical & Procedural Equipment
Surgical and procedural tools are essential for specialists and ambulatory surgery centers.
Commonly financed equipment includes:
- Surgical tables
- Laparoscopic towers
- Endoscopy systems
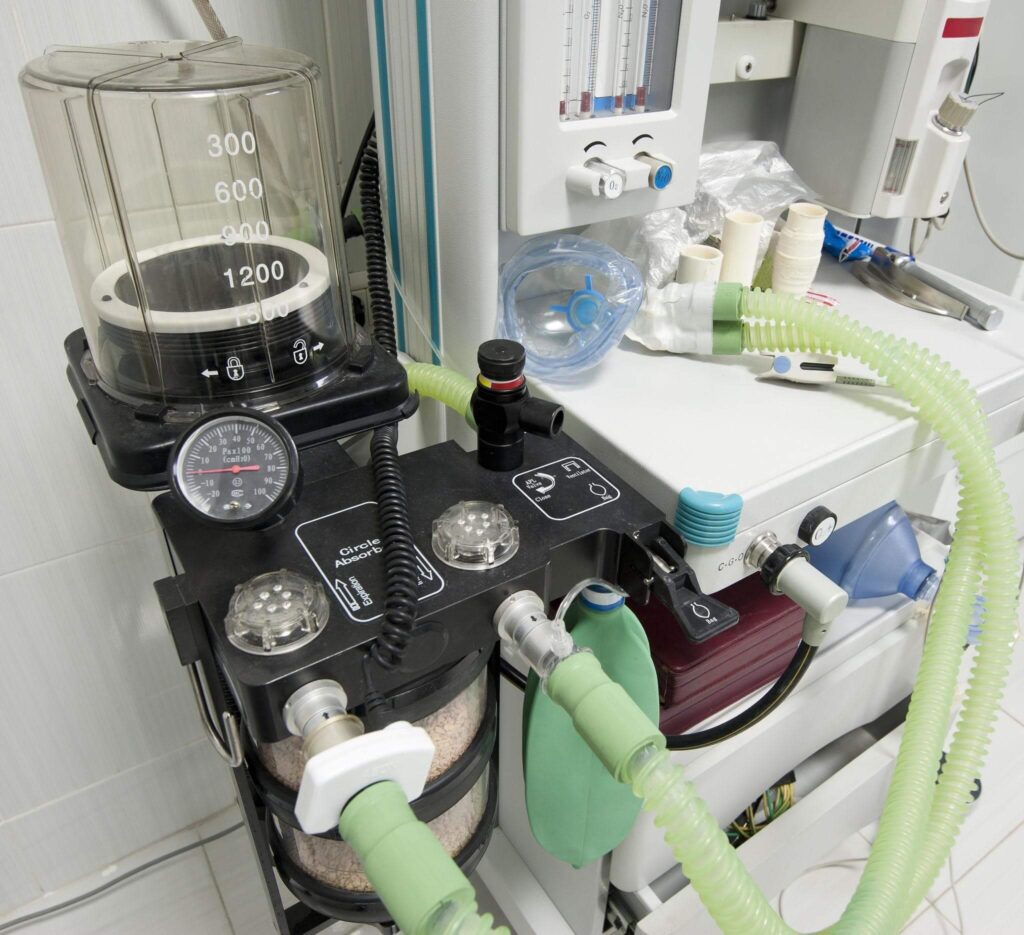
- Anesthesia machines
- Patient monitoring systems
These assets are expensive but directly tied to revenue-producing procedures.
Medical equipment financing in this category typically involves:
- Equipment loans with fixed rates
- Capital leases
- Operating leases for rapidly evolving technology
Because surgical systems can become outdated, many physicians prefer lease structures that allow upgrades every few years.
Dental & Specialty Equipment
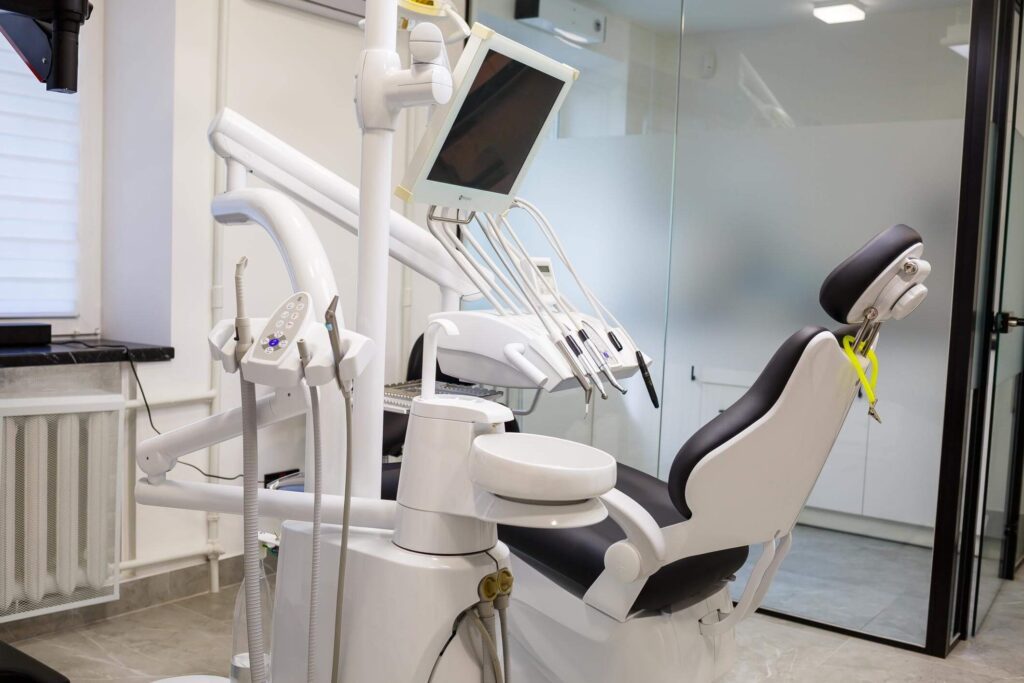
Dentists, dermatologists, ophthalmologists, and other specialists frequently use medical equipment financing to build out high-tech treatment rooms.
Examples:
- Dental chairs and digital imaging
- CAD/CAM systems
- Dermatology laser platforms
- Ophthalmology diagnostic tools
Dental equipment financing is especially common when launching a new practice. Entire operatories are often bundled into a single financing package.
Because these specialties often operate on fee-for-service or partially cash-based models, equipment ROI can be easier to forecast compared to insurance-heavy practices.
IT Systems & Electronic Health Records
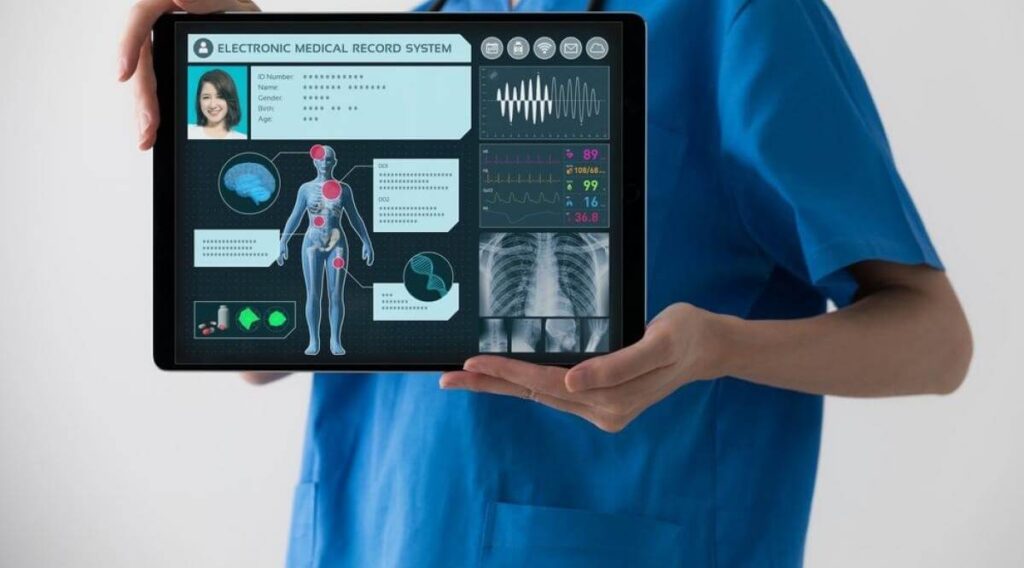
Medical equipment financing isn’t limited to physical machines.
Doctors frequently finance:
- Electronic Health Record (EHR) systems
- Practice management software
- Telemedicine infrastructure
- Server and data storage hardware
Digital systems are essential for compliance, billing efficiency, and patient communication.
Because software evolves quickly, leasing or subscription-based financing models often make more sense than outright purchases.
Facility & Infrastructure Equipment
When opening or expanding a practice, doctors also finance:
- Exam tables
- Autoclaves
- Sterilization units
- Medical-grade HVAC systems
- Built-in cabinetry and casework
While less glamorous than MRI machines, this equipment is necessary for compliance and patient safety.
Medical equipment financing for infrastructure is often bundled into startup practice loans or SBA-backed financing programs.
Trade-offs: The True Cost of Medical Equipment Financing
Interest Rates: Loan vs Lease
With medical equipment financing, you typically choose between:
- Term loan (you own the equipment)
- Capital lease (ownership transfers at end)
- Operating lease (return or upgrade at end)
Loans build equity but may carry longer obligations.
Leases offer flexibility but can cost more over time.
Interest rates depend on:
- Credit profile
- Practice revenue
- Equipment type
- Loan term length
Healthcare is often considered lower-risk lending, so doctors frequently receive competitive rates compared to other industries.
Technology Obsolescence
Medical innovation moves fast. A machine that is cutting-edge today may be outdated in five years.
This makes long-term financing risky for rapidly evolving technologies like:
- Imaging systems
- Laser platforms
- Software systems
Medical equipment financing terms should align with realistic equipment lifespan.
Cash Flow & Reimbursement Risk
Insurance reimbursement delays can disrupt predictable revenue.
If payments from Medicare or private insurers are slow, fixed loan payments still must be made.
Smart medical equipment financing aligns monthly payments with expected revenue per procedure, building in buffer for reimbursement delays.
Tax Strategy & Depreciation
Under U.S. tax law, physicians may deduct equipment purchases through depreciation or Section 179 (subject to limits and changes).
Medical equipment financing can enhance tax efficiency because:
- You may deduct interest
- You may depreciate the full equipment cost
- Lease payments may be deductible as operating expenses
Always consult a healthcare-focused CPA before structuring large financing deals.
Next Steps: How Doctors Should Approach Financing
Step-by-Step Evaluation Framework
- Calculate projected procedure volume
- Estimate reimbursement per procedure
- Subtract operating costs
- Ensure payment-to-revenue ratio is conservative
- Compare loan vs lease offers
- Stress-test cash flow under slower patient volume

Startup Practice Example
A physician opening a family medicine clinic may need:
- Exam tables
- EHR system
- Basic diagnostic tools
- Ultrasound machine
Instead of paying $250,000+ upfront, the doctor bundles equipment into a startup loan backed by programs supported through the U.S. Small Business Administration.
Monthly payments are structured over 7–10 years, preserving cash for payroll and marketing.
Established Practice Expansion Example
A cardiology practice wants to add advanced imaging to keep referrals in-house.
By using medical equipment financing structured over 5 years, the practice matches monthly payments to anticipated imaging revenue.
If imaging volume meets projections, the equipment becomes a high-margin asset after payoff.
If not, the debt can strain operations.
That’s why conservative forecasting is essential.
Making Medical Equipment Financing Work for You
Medical equipment financing isn’t just about getting approved.
It’s about aligning:
- Equipment lifespan
- Revenue generation
- Cash flow stability
- Tax strategy
- Long-term growth goals
Before signing any agreement:
- Get multiple quotes
- Review effective APR
- Understand prepayment terms
- Stress-test revenue assumptions
When structured properly, medical equipment financing allows doctors to deliver better care, expand services, and grow profitable, modern practices—without jeopardizing financial stability.
Q1: Do most doctors finance medical equipment?
Yes. Because equipment is expensive and revenue-generating, medical equipment financing is standard practice in both small clinics and large healthcare systems.
Q2: Is leasing better than buying?
It depends on technology lifecycle. Rapidly evolving equipment often favors leasing. Long-lasting infrastructure may favor purchasing with financing.
Q3: Can new doctors qualify for financing?
Yes. Lenders often consider medical degrees and projected income highly favorable, especially with SBA-backed support.



No comment